A cycling accident. The loss of a beloved grandmother. A career-ending sports injury. These University of Florida researchers are united by deeply personal experiences that motivate them to understand the brain — and make it work better amid disease or injury.
Mapping the brain—and a path back from her own injury
Even after years of studying deep brain stimulation, what fascinates Aysegul Gunduz the most is the brain’s ability to adapt — to allow artificial electrical current to alter cell activity and quell tremors or tics, seizures or involuntary muscle contractions.
“People say you can’t teach an old dog new tricks, but you really can,” says Gunduz, a biomedical engineer and director of UF’s Brain Mapping Laboratory.
Three and a half years ago, her longstanding appreciation of the brain’s plasticity was put to the test: She herself was wheeled in under the bright lights, her brain the one to be operated on.
She had been training for a triathlon on a new bicycle when she suddenly hit a rough patch of pavement, lost control and fell. Although she was wearing a helmet, the impact caused a traumatic brain injury and a need for emergency surgery to relieve pressure in her head and stop seizures.
Dr. Brian Hoh, chair of UF neurosurgery, performed the operation. The days before and after were a blur to her, but one thing she knew in her heart, she says: “I owe him my life.”
Every day in intensive care, she was visited by her longtime collaborators Dr. Michael Okun, a neurologist, and Dr. Kelly Foote, a neurosurgeon. A decade earlier, Okun and Foote, now co-directors of the Fixel Institute, had been searching for an expert who could analyze brain signals in their pursuit of continuing to improve deep brain stimulation for Parkinson’s disease and other conditions. They’d been working as a team ever since.
“She is creative, she is innovative, and she is brilliant,” Okun says. “She’s an expert at taking the language of the brain and converting it into units that we can use to decode certain symptoms and develop therapies.”
Gunduz sensed quickly it was the right fit. “Sometimes clinicians think engineers are like technicians who magically put together the things they want,” she says with a chuckle. “But Mike and Kelly gave me an equal seat at the table. They lift up people around them.”
Years later, as she healed from the accident, support and encouragement from many — her fiancé (now husband), colleagues and family back in Turkey — helped her get back on track. Care by UF neuropsychologist Russell Bauer, an expert in traumatic brain injury, and the UF Health rehab team helped her get back to work and fueled her determination.
Over time, her perspective on the accident has evolved. “As ironic as it is for this to happen to a brain researcher, I knew my brain could regain the functions that were impaired,” says Gunduz, whose many awards over the years include the Gator Nation Leadership Award and the Presidential Early Career Award for Scientists and Engineers, the highest honor given by the U.S. government to outstanding scientists and engineers beginning independent careers.

“Having worked with a lot of neurosurgical patients, I knew that if you keep at it, your brain can heal itself,” she says. “So that kept me going, as well as the promise I had to my Ph.D. students. And my father is a physical medicine rehabilitation doctor back in Turkey, so that kept me going, too.”
All along, she held onto a deep belief in her capacity to grow, a belief that stretched back to her school days, when a teacher once told her, “I don’t see you becoming an engineer.” After initial tears, she didn’t give up, and in summer 2023 she shared the teacher’s words on social media on the day she was promoted to full professor of biomedical engineering.
Her determination to recover from the accident and get back to her research was no surprise to longtime colleagues such as Peter Brunner, who worked with Gunduz during her postdoctoral fellowship at Albany Medical College in 2011.
“She not only made a remarkable recovery, but she also has gained extremely valuable insight for herself on how the human brain is plastic and how it can recover,” says Brunner, an associate professor of neurosurgery and biomedical engineering at Washington University in St. Louis. “This is really a compliment to all the physicians involved in her recovery but also to her perseverance and strong push to move forward.”
Not only did she make it through, he says, but “she came back out on the other side even stronger.”
Brunner saw the same spark in her at the start of her career, when she chose to pursue a line of technological research considered risky at the time: detecting debilitating tics, which then was seen as the cutting edge of what scientists thought could be done.
“She picked something that’s really difficult and literally bet the farm on it,” Brunner says. “She picked something nobody really saw taking off and was extremely successful and developed herself into one of the world experts in deep brain stimulation.”
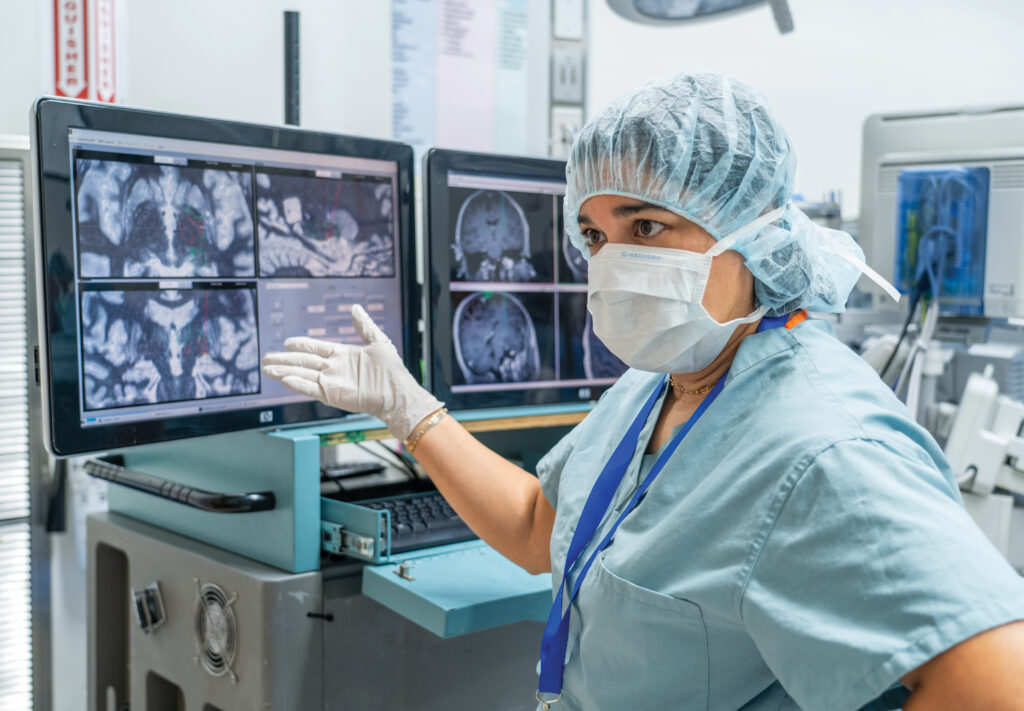
Today, Gunduz, the inaugural Fixel Brain Mapping Professor, is back in the operating room at the UF Health Neuromedicine Hospital. With MRI images on a monitor beside her, she watches as innovative software she developed is used in patients undergoing deep brain stimulation (DBS) surgery to ease symptoms in conditions including Tourette syndrome and essential tremor.
Her current focus is to make DBS more like a cardiac pacemaker, in a way — to make the mild pulses of electricity responsive to changing signals in the brain rather than continuous, to limit side effects and the draining of the implant’s battery.
Some days in the operating room, the team uses software she developed to map the brain of a patient to guide implantation of an electrode. Other days, she is collecting neurophysiological data, for later decoding of brain signals to refine aspects of DBS and develop the next generation of software.
“She is guiding the future,” says Okun, “of how the brain is going to be targeted and how we’re going to intervene.”
Moving toward a broader view of Parkinson’s
Dr. Ashley Rawls looks out at her audience and asks: When you hear “Parkinson’s disease,” who is the first person you see in your mind?
“Michael J. Fox,” responds one participant. “Janet Reno,” says another.
Rawls then projects a photo of Muhammad Ali. In unison, several utter his name. Nodding along, Rawls says, “It affects a multitude of people from different backgrounds.”
A UF Health neurologist and researcher who specializes in movement disorders, Rawls is helping spread the message that Parkinson’s reaches across races in hopes of getting more patients diagnosed earlier and providing better access to care. One strategy to do this has been free community events like this one, sponsored by the Parkinson’s Foundation, to chip away at common misconceptions of who is a typical Parkinson’s patient.
“If you search online for Parkinson’s, one of the first images you see is this older white gentleman who’s hunched over with tremors,” says Heather Simpson, a UF Health occupational therapist and a co-leader of the community outreach efforts. “In particular within the African American and Black community, many of the Parkinson’s symptoms can be misconstrued for typical aging, such as heart disease and diabetes.”
Every year, approximately 90,000 Americans receive a new Parkinson’s diagnosis, according to the Parkinson’s Foundation, and 1.2 million are projected to be living with the condition by 2030. But according to a review of medical literature, research has shown that African American patients diagnosed with Parkinson’s are less likely to receive standard of care than white patients and more likely to come to specialty clinics with severe or advanced disease, and one study looking at the largest group of Black Parkinson’s patients from a single center, in Chicago, showed they were four years older at first diagnosis.
In Gainesville, the initiative of one patient who sought to help others deeply moved Rawls.
At first, Orien Greene, a UF Health neurology patient, thought his stiffness and slowness were arthritis and his insomnia was due to the stress of a rough day. But after getting a Parkinson’s diagnosis two years ago, he came up with the idea of doing community outreach, and together, he, Rawls and Simpson hatched a plan. Last year, with a $9,430 grant from the Parkinson’s Foundation, they brought the “Power in Knowing” program, a partnership with the Norman Fixel Institute for Neurological Diseases at UF Health, to assemblies at two churches and one school in the Gainesville area.

“The sooner you catch it, the better it is with most medical things, and likewise with Parkinson’s,” says Greene, 67, who early on kept his diagnosis private. “I wrestled with that for a minute, but then I made the decision that, OK, it’s better to let people know, not just harbor the information, and maybe it’ll help somebody else as well.”
The team was encouraged by response to their program: Surveys showed an 83% improvement in knowledge of Parkinson’s symptoms, a 118% improvement in knowledge of treatment options and a 148% improvement in knowledge of where to go for patient and family resources, on a 4-point Likert rating scale, Simpson says.
“Dr. Rawls knew what the community needed,” Simpson says. “She can communicate from personal experience, which is very helpful, and she’s a very trustworthy and caring person.”
As a medical school student, Rawls witnessed firsthand the health problems facing her maternal grandmother and lapses in communication between doctors and family members at a time when trust was needed and worries ran high. Her mother was a science teacher and her father a nuclear engineer, but medical jargon leaves a lot of room for miscommunication for almost everybody, she says.
“I found that there’s this divide between all the things that medical personnel are trained with and know and being able to converse and talk with people who may not have the same level of expertise,” she says. “There was a breakdown there. So one thing that brought me toward medicine is trying to bridge that gap in communication.”
The death of her beloved grandma, known as “Ms. George,” in her fourth year at the UF College of Medicine further inspired Rawls’ drive to teach medical students. Following residency at the Medical University of South Carolina and a fellowship in movement disorders at Stanford, Rawls returned to UF as a clinical assistant professor. In addition to teaching and caring for patients, she is also the site principal investigator of a national clinical study, Black and African American Connections to Parkinson’s Disease, known as BLAAC PD.
The six-site study, a partnership of the Aligning Science Across Parkinson’s initiative and The Michael J. Fox Foundation for Parkinson’s Research, is examining the genetics of Parkinson’s, identifying similarities and differences among different ethnic heritages. At UF, BLAAC PD study participants, both with and without Parkinson’s disease, contribute an anonymous one-time blood or saliva sample for DNA testing as well as demographic and family medical history.
“About 90% of genetic studies performed in the Parkinson’s field are persons of European ancestry, so the genetic impact of PD susceptibility on Black and African American populations is largely unknown,” Rawls says. “BLAAC PD will help us learn about the potential linkage between genes and our patients of Black and African American descent.”
Her greatest hope is that by understanding the factors that contribute to Parkinson’s, this will yield new focused treatments in the future.
Sidelined by concussions, she now studies new treatments
Sledding belly-down and head-first on an ice track at 70 miles per hour day after day, Aliyah Snyder could feel her chin and the side of her head vibrating against the ice. She was on the rise in the sport of skeleton, ranked 44th in the world and competing on the North America’s Cup circuit, when persistent headaches, dizziness and loss of balance forced her to step away.
This was before there was increased awareness nationally about concussions, she says, before “getting your bell rung” meant something potentially more serious. During her yearlong recovery back home in the Florida Panhandle in 2010, she kept thinking about research-assistant work she did as an undergrad at the Florida Institute of Technology, looking at soccer heading and potential risks of concussion and neurocognitive impairment. As she bounced from medical appointment to appointment, she had a revelation.
“There was a lack of effective health care and education around concussion,” Snyder says. “I thought: This is meaningful to me. There is clearly a huge gap in health care that I can contribute to.”
The daughter of an Air Force pilot and a satellite meteorologist, Snyder grew up moving across the U.S. and first showed her athletic ability in high school, when she was a Florida state fencing champion three years in a row. Fast forward to post-college, she was assistant coach of the men’s rowing team at Connecticut College when a boyfriend who was training on the bobsledding team at the Olympic Center suggested she try skeleton. She thought it looked crazy and, as an adventure seeker, like a lot of fun.
“I remember the first time I went off the top of the track in Lake Placid, and you know you’re going to hit 70 miles an hour — nothing’s going to stop you from hitting that speed, and like, buckle up,” she says, laughing. “It’s like flying. It’s the biggest adrenaline rush I think there is.”

She trained for two years, earning a spot on the Israeli national team, before the constant subconcussive impact of her head knocking against the ice became too much. Once back at home in Florida, she reached out to her Florida Tech mentor Frank Webbe, a triple-Gator with a doctorate in psychology from UF and an expert in sports-related brain injury. Could she come back to his lab, as a volunteer? He didn’t hesitate.
“She was on a mission,” Webbe says. “And that mission was to put people in touch with knowledge and with contacts that would help them, and it was also to create new knowledge to help them.”
Early on, he could see she remained concerned about some lingering symptoms of her own, but as the symptoms improved, she embraced new academic and research projects. In addition to analyzing data, she began creating websites and programs for people who’d had brain injuries and then decided to apply to graduate school in neuropsychology at UF.
She wanted to focus on persisting symptoms after concussion, an area of study that has been under-researched, says Russell Bauer, professor emeritus of clinical and health psychology who became her UF mentor. This allowed Snyder to stake out her own territory.
“Her situation fits to a T with what she’s interested in studying, because she did not have an ‘incident concussion’ where she banged her head and lost consciousness,” Bauer says. “Her concussions resulted from chronic subconcussive jostling of the head from going down the track.”
For her dissertation, she took the rare approach of running a clinical trial. Her goal was to examine the effects of aerobic exercise on concussion recovery, in light of conventional wisdom to only rest after concussion. In her pilot study of 26 young-adult participants who were 14 to 25 days post-concussion, Snyder found a one-week aerobic exercise program didn’t appear to negatively impact cognition, mood, sleep or neurocognitive performance.
After internship training at Emory in pediatric and adult rehabilitation neuropsychology and a fellowship at UCLA in brain injury and sports neuropsychology, Snyder returned to UF in 2020 as an assistant professor and clinician-researcher in the College of Public Health and Health Professions. Today she’s part of an interdisciplinary team that specializes in concussion assessment and treatment, and she directs the Holistic Interventions for Brain Health and Recovery Clinic, with techniques including psychotherapy, mindfulness meditation and biofeedback.
“She’s developed a multi-pronged approach to identifying and then treating these symptoms, which include hypervigilance, autonomic hyperarousal, sleep disturbances, depression — each has a biological component and also a psychological component,” Bauer says. “She’s implementing very specific targeted interventions for each of those areas.”
Snyder also maintains a position as a project scientist for the UCLA Steve Tisch BrainSPORT Program, and in that role, she’s currently running an arm of a large multisite NIH-funded study into pediatric concussion recovery, the CARE4Kids study. The study includes patients ages 11 to 17 who have been diagnosed with a concussion, and Snyder’s part is to oversee autonomic assessment. She is tracking measures such as heartrate variability, or the variation in time between each heartbeat, while collaborators are collecting blood and advanced neuroimaging, among other techniques, to predict which children will develop persistent symptoms.
In another project, Snyder plans to expand a UF interdisciplinary concussion database to track outcomes of various interventions, to better understand the efficacy of current treatments and design future trials to test new approaches, such as vagal nerve stimulation.
Overall, what she hopes to achieve is widespread availability of specific interventions to help people recover, starting with a standardized, self-paced online program she plans to develop.
Snyder says her personal experiences with concussion and with long COVID — a new area of study for her — drive her on a daily basis.
“Everybody’s journey is very different, but I empathize with every patient coming in and going through recovery,” she says. “What I relate to most is the search for answers, and we are finally coming to a place where we have more answers.”
It’s still ambiguous in many areas, she says. “But to give some type of empowerment or control back to patients in their recovery — that’s where I get the most satisfaction.”

Sources:
Aysegul Gunduz
Professor of Biomedical Engineering and Fixel Brain Mapping Professor
agunduz@bme.ufl.edu
Ashley E. Rawls
Assistant Professor of Neurology
ashley.rawls@neurology.ufl.edu
Aliyah R. Snyder
Clinical Assistant Professor of Clinical Health and Psychology
aliyahsnyder@ufl.edu