As coronavirus cases headed for a peak globally, the world went on a scavenger hunt for ventilators, the expensive breathing machines that keep the sickest patients alive. But keeping the ventilators going requires parts to connect them to patients.
“Suddenly, that humble piece of plastic tubing that you almost didn’t acknowledge existed is the center of your patient care universe,” says Dr. Lars Beattie, the director of the emergency medicine residency program at the University of Florida.
Plastic tubing, cotton swabs, face masks, surgical gowns, gloves, test tubes, chemicals for testing, medications for treatment – all these components are part of a complicated health care supply chain that already had some weaknesses before the pandemic, says Elif Akcali, an associate professor of industrial and systems engineering in UF’s Herbert Wertheim College of Engineering.
Common disruptions in a supply chain can stem from a temporary shortfall in a raw material. More severe disruptions can occur after a natural disaster. A hurricane, for example, can cause disruptions to supplies in the area hit, but that area can be rescued by supplies shipped in from the outside. The difference in the pandemic is that global supply chains buckled in a cascading fashion. Starting in the Far East, the virus – and the shortages – rolled toward Europe and then the United States and South America. As the supply chains in manufacturing centers in the Far East broke down, other countries could not step up to fill the gap.

“Typically, one node of a supply chain might break down and then recover, or if there’s a shortage in one area, someone from another area helps,” says Akcali, the Cottmeyer Family Innovative Frontier Faculty Fellow.
“This was the Black Swan event no one could foresee.”
Making the health care supply chain more resilient is the goal of a research team Akcali has assembled, including Beattie and other doctors and health care administrators.
Pharmaceutical Supplies
Akcali says the slowdown in supplies of common drugs and chemical reagents critical in medical testing occurred early as the coronavirus took hold in China. Another core pharmaceutical manufacturing area was in Lombardy, the region of Italy with the highest concentration of coronavirus cases.
“Lombardy and China provide medications and critical reagents for the rest of the world and they were hard hit very early,” says Akcali.
Akcali says of 156 generic drugs – like blood pressure medications or antibiotics – the critical ingredients for 85 percent of them are manufactured outside the U.S., mostly in China. As of March 30, there was a two- to three-month supply of most of these common medications, but that quickly dwindled.
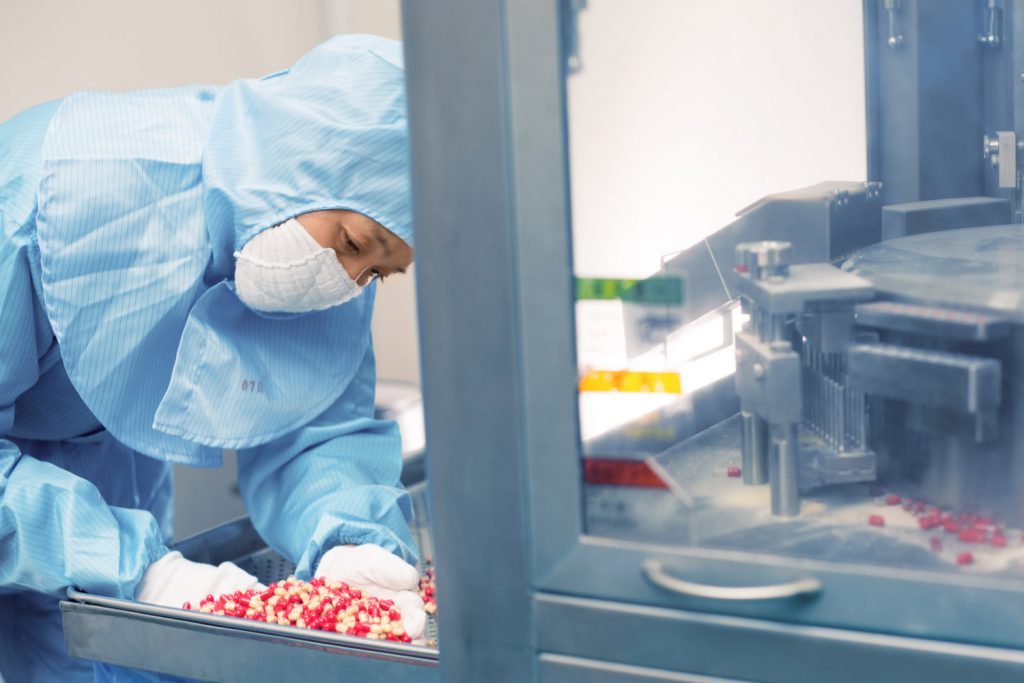
“We use these on such a regular basis that we don’t even think about them,” Akcali says.
Dr. Rosemarie Fernandez, a clinical associate professor of emergency medicine, says doctors are accustomed to periodic shortages and adept at changing patient treatment protocols. COVID-19 made that more challenging.
“There’s always a cyclical thing that happens with medications, but I think we’re feeling it a little more now,” Fernandez says. “Your first-line medication might be gone, but the second line medication is gone, too, so you’re reaching deeper and deeper down the list.”
Before coronavirus, a patient going into an ICU might stay for three or four days, using a three- or four-day supply of sedation, medications and IV antibiotics, Akcali says. With coronavirus, patients can stay in the ICU much longer, an average of 11 or 12 days, creating a need not only for medications but also for equipment like ventilators. Demand went up just as supply constricted, she says.
“We’ve been seeing a shift in attention for some of these pharmaceutical and health care products that were kind of under the radar,” Akcali says.
Beattie agrees, and says the keen interest in personal protective equipment, or PPE, is warranted: “With COVID-19, PPE is essential in caring for these patients.”

Personal Protective Equipment
When Akcali began looking into the health care supply chain in December, she met with UF hospital administrators in charge of strategic sourcing. Akcali asked, “What’s keeping you up at night; what problem do you want to solve?”
Administrators, concerned about the annual flu season at that time, replied that they were concerned that there are only five suppliers inside the United States for surgical gowns and other personal protective equipment.
To minimize costs, most companies, including hospitals, try to identify a single supplier for a product and buy in bulk. If that supply is disrupted, identifying an alternate source may not be sufficient.
The alternate supplier may not welcome the extra business because if it meets a new customer’s needs, it might have to “starve regular customers,” Akcali says.
Companies that have experienced severe disruptions, such as Toyota following the Japanese tsunami in 2011, have diversified their supply chains, Akcali says, and health care may need to follow suit.
Following the tsunami, Toyota reinvented its supply chain, adopting a 50-30-20 percent supply plan. It buys 50 percent of its materials from its preferred supplier but also buys from two other suppliers, so that alternative sources for materials exist.

If demand for PPE spikes again, it may be critical to identify new sources. The monthly output of PPE manufacturers in the U.S. is only enough to supply a large emergency medicine department in New York City for one week, Akcali says.
“The output doesn’t start to meet the demand,” Akcali says.
When demand spiked as coronavirus cases grew, the situation became challenging, Fernandez says. Masks that used to be everywhere suddenly were in short supply.
“These masks that were part of our everyday weren’t there,” says Fernandez, who procured some of her own PPE on eBay. “It happened so fast; where did they go?”
Beattie, who oversees residents, said the emergency department has been able to stay within Centers for Disease Control and Prevention guidelines on use and re-use of PPE, but even today he hangs on to his used masks, with some in “semi-retirement.”
“It’s a different situation today, but heading into this, it was a little frightening to think of not having the PPE,” Beattie says.
Beattie and Fernandez say they are looking forward to helping Akcali model what has already happened and ways to prevent disruptions in the future.
“Understanding the supply chain itself and the weak point for future high-pressure situations that require a lot of PPE will help us direct efforts toward supply chain resilience and shore up the weak points,” Beattie says.
Back to the Basics
In her research, Akcali wants to tackle two things: supply chain agility and resilience. Sourcing, she says, is critical to both.
“How do we change our sourcing strategies so that we adapt quickly to changes in the environment?”
Resilience and agility may require health care enterprises to shift from volume-based contracts to contracts that have emergency contingencies. Some companies achieve this by identifying alternative suppliers and buying the right to purchase a product at a point in the future under certain conditions. The buyer pays a fee and the supplier commits to providing goods when needed. Companies benefit by not having to keep inventory on hand, and suppliers benefit from an incentive, the slightly higher price.
Supply chain transparency can help, too. Akcali says even a buyer who identifies two suppliers can come up short if the buyer does not know that both suppliers are using the same source for materials. It’s important for a buyer to ask where all the materials that go into a product are coming from. For example, if a hospital has two suppliers for face masks, if both suppliers are getting the fabric for the masks from the same supplier, the supply chain is still vulnerable if the fabric company experiences a shortage.
“We need transparency that goes back three or four levels,” Akcali says. “At no point in time should I make myself reliant on a single source, because if that one source disappears, what am I left with?”
Minimizing costs also ignores other supply chain considerations, such as protecting human assets.

“What we’re seeing now is that some of those items no one paid attention to because they were cheap and readily available, now those are becoming critical supply items,” Akcali says. “We may have to become more comfortable operating at a higher cost, to be sure we are ready for something like this. You don’t want your peak capacity to come down to PPE.”
Alachua County and UF Health were spared the brunt of the pandemic. The Florida Department of Health listed 88 hospitalizations and 10 deaths in Alachua County as of June 15. Both Beattie and Fernandez have colleagues who saw the pandemic at full force. Beattie’s previous hospital was Elmhurst in Queens, which was ground zero in the United States, and Fernandez came to UF from Seattle, not far from where the first U.S. coronavirus case was diagnosed.
“We still have to be hypervigilant,” Fernandez says. “It’s possible the worst has not hit us yet.”
Both are looking forward to contributing a boots-on-the-ground view for Akcali’s research.
“A deep analysis of what’s happening will really inform us of how to respond better next time,” Beattie says.
Akcali agrees: “The next time, the next pandemic, we want to have checks and balances in place.”
Akcali says she has been surprised at hearing so many people talking about supply chains in the past few months. She says she was concerned that artificial intelligence and machine learning might reduce the importance of supply chain research.
“Now everyone knows about supply chains,” Akcali says. “You hear the phrase ‘supply chain’ multiple times a day. That’s really unprecedented for us.”
Sources:
Elif Akcali, Associate Professor of industrial and systems engineering
Rosemarie Fernandez, Clinical Associate Professor in emergency medicine
Lars Beattie, Emergency Medicine Residency Program Director

